A study looking at 15 years of HIV transmission and suppression in Uganda reveals how closing gender gaps in treatment could slash infection rates.
Providing more heterosexual men with easy access to HIV treatment and care could help to suppress the virus and rapidly cut transmission to their female partners, shows a new study published in Nature Microbiology.
The research, led by scientists from Imperial College London and the Rakai Health Sciences Program (RHSP) in Uganda, analyzed 15 years of data from 2003-2018, during which the US President’s Emergency Plan For AIDS Relief (PEPFAR) has delivered an extensive program of HIV/AIDS testing, prevention, and treatment.
This included distributing Antiretroviral Therapy (ART) drugs, which suppress the virus so a person is no longer infectious. The analysis shows that the PEPFAR program and other services have greatly reduced new infections among young women and heterosexual men but that reductions were less substantial in women aged 25 and above.
This is thought to be because women are more likely to reach viral suppression through uptake and effective use of HIV treatment, preventing them from passing HIV to their male partners, but the same is not true the other way around.
Gender disparity
The analysis showed that the number of women reaching and maintaining undetectable (non-transmissible) levels of HIV infection were 1.5 to 2 times higher than men across all ages by the year 2018. The analysis shows that had men reached the same levels of virus suppression as women, around half the new infections that occurred between 2016 and 2018 could have been avoided.
The team also reconstructed transmission networks based on the genetic code of the virus from thousands of participants, which confirmed that overall, the proportion of transmissions from men is increasing and is now at 63% of all transmissions in the area—even though a greater number of women are living with HIV than men.
The team says the disparity could be because men need to travel for work, that clinics are closed when they are back home, or for other reasons, including social stigma.
Dr. Oliver Ratmann, senior author of the study from the Department of Mathematics at Imperial, said, “In this evolving battle against HIV, it is critical we adapt our strategies, bridge gaps in care, and ensure that individuals, regardless of their gender, have access to the lifesaving benefits of ART.
“It is important to design services in a way that everybody who would like to use them is able and feels empowered to do so. By routinely monitoring the changing dynamics of the epidemic and striving for equity in HIV care, we can move closer to the ultimate goal of controlling and, one day, eliminating HIV transmission.”
Dr. Kate Grabowski, a co-author of the study from the Johns Hopkins School of Medicine, added, “The continued success of the President’s Emergency Plan for AIDS Relief (PEPFAR) in reducing infections and saving lives is crucial for ending HIV transmission.”
“With United States Congress currently evaluating PEPFAR funding, our evidence strongly supports the program’s efficacy and provides a clear roadmap to ending the pandemic through enhanced HIV treatment coverage, particularly among men.”
Closing the gap in transmission
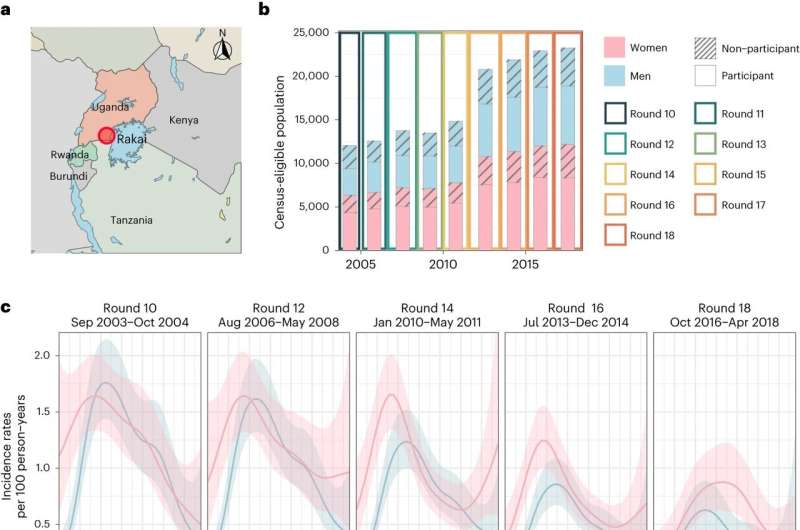
The team used data from the Rakai Community Cohort Study (RCCS) in southern Uganda, a region where more than 9% of adults are living with HIV—approximately 20 times higher than in the US. Since 2003, a period predating the widespread availability of ART in Africa, RCCS has enrolled nearly 37,000 individuals, tracking changes in HIV infection as new interventions came on board.
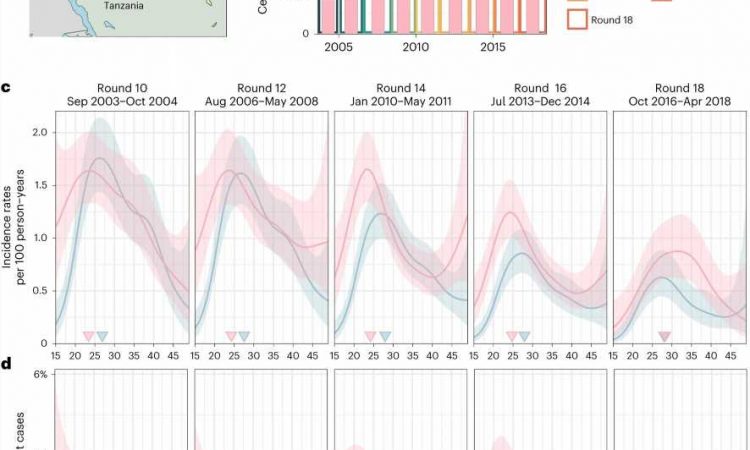
The analysis tracked evolving heterosexual HIV epidemic dynamics in 36 communities over a 15-year span of RCCS surveillance data, including records of new infections, deep sequence HIV genomic data, HIV treatment uptake, viral suppression, and behavioral information.
Analyses in earlier years showed that the highest number of new HIV cases in southern Uganda was among adolescent girls and young women aged 15-24 years. In more recent years tracked in the new study, women 25-34 years old have become a new focal group, experiencing a slower decline in new infections than other age groups. This is alongside a significant difference in the declines in new infections between men and women, with those among boys and men declining much faster.
To estimate the likely impact of getting men to the same level of viral suppression, the team applied statistical models based on the data about transmission dynamics. The resulting projections indicate that closing the viral suppression gap in men could have effectively halved rates of new infections among women and eliminated gender disparities in acquiring HIV.
Dr. Joseph Kagaayi, previous director of the Rakai Health Sciences program and senior co-author of the study, said, “Our study findings emphasize the importance of addressing disparities in ART uptake and viral suppression between men and women. By doing so, we can not only reduce HIV infections among women but also work towards closing the gender gap in HIV transmission. Achieving these goals will require concerted efforts, informed policies, and strengthened health care services.”
More information:
Mélodie Monod et al, Longitudinal population-level HIV epidemiologic and genomic surveillance highlights growing gender disparity of HIV transmission in Uganda, Nature Microbiology (2023). DOI: 10.1038/s41564-023-01530-8
Journal information:
Nature Microbiology
Source: Read Full Article