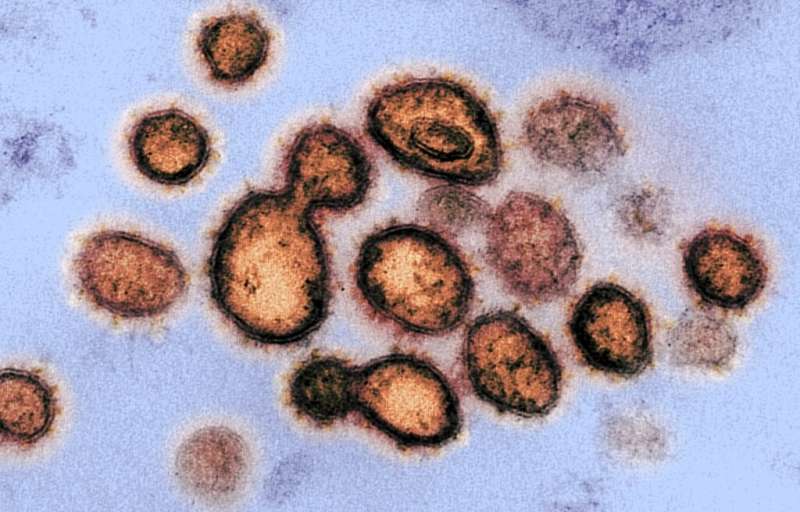
The emergence of several, more infectious strains of the novel coronavirus SARS-CoV-2 has worried governments and scientists, who are investigating how and why the virus became more transmissible.
Like all viruses, SARS-CoV-2 mutates in order to maximise its survival chances.
When it replicates, tiny errors in its genetic coding are introduced.
Most of these are inconsequential. But some—as with the virus variants that emerged recently in Britain, South Africa and Brazil—can give the virus a decisive new advantage.
“When we keep case numbers high, we are maximising the virus’s opportunities to get into weird situations, that might be rare, and most of them might lead nowhere,” said Emma Hodcroft, epidemiologist at the University of Bern.
More cases equal more transmissions, which maximises the chances that a significant mutation will occur, she said.
“If we keep case numbers lower, we essentially restrict the virus’s playground.”
Wendy Barclay, a virologist at London’s Imperial College, said mutations were a result of several factors.
“It’s a combination of how much virus is out there, the number of times you roll the dice defines what happen, coupled with the environment the virus is currently in,” she said.
It was not unexpected for the new variants to appear after a year of COVID-19 as levels of global immunity increase through vaccinations and natural infection, she added.
“In South Africa and Brazil there was already quite a high level of antibody response from people who had been infected and recovered from the virus.”
‘Immune pressure’
Other experts expressed doubt that immunity levels directly influenced the current mutations.
Bjorn Meyer, a virologist at the Institut Pasteur in Paris, said it was more likely each mutation occurred in a single individual, who then passed it on to others.
He explained the possibility of a patient whose immune system was compromised, and therefore unable to clear the virus as quick as others.

“In this patient there might be something defective in the response so the virus can just stay around for a long time,” Meyer told AFP.
While the COVID-19 virus typically infects individuals for around 10 days before being neutralised by the body, some studies have shown that certain patients may carry it for several weeks or longer—maximising the window for mutations.
“There is still some level of immune pressure on the virus in this patient and the virus is being forced to mutate,” said Meyer.
He said a more transmissible variant was likely to develop only later during the pandemic, as most immunosuppressed individuals had been shielded for months and so few would initially have been infected.
But as cases rise, the chance of the virus infecting an immunosuppressed patient—and therein mutating significantly—also grows.
More variants?
Immune issues may also have impacted the virus in another way.
France’s Academy of Medicine says that the South African variant “could result from a viral replication more intense and prolonged in people living with HIV”—cases of which are highly prevalent there.
While the precise origins of the variants remain up for debate, scientists are unanimous that their effect needs careful management.
A more transmissible strain of the virus has been blamed on a surge in COVID-19 cases and deaths in Britain.
Although more infectious, there is currently no evidence to suggest the new variants are more virulent than other forms of SARS-CoV-2.
“One can’t rule this risk out,” said Meyer.
But with the current sanitary and distancing measures in place around the world, coupled with vaccination campaigns, the virus’ “selection pressure” is likely to affect transmissibility rather than potency, he added.
One thing is for sure: the virus will continue to mutate, which might bring more dangerous variants.
In fact, they may already be circulating.
Source: Read Full Article
