Women around the world who have positive health ‘reparations’ during the journey through pregnancy benefit throughout their lives, new research says.
In a new paper published in eClinicalMedicine as part of a special World Health Organization series on maternal health, academics review existing theories of ‘vulnerability’ for women during pregnancy and the impact that reparative strategies have on long-term health, including for future pregnancies.
The team, led by Professor Shakila Thangaratinam from the University of Birmingham, argues for reshaping the concept of ‘vulnerability’ in maternal health, making a case for a preventative, holistic approach to good health for women and girls, including proactively identifying vulnerability and promoting customized care plans in maternity settings around the world.
Professor Shakila Thangaratinam, Joint Director of WHO Collaborating Centre for Global Women’s Health at the University of Birmingham and lead author of the second paper in the series, said, “It is possible to reverse damages to a mother’s health that she may experience throughout the pregnancy journey through reparative strategies. Each time there is a reparative strategy that happens in pregnancy, birth, and beyond, it pulls the woman toward ideal health. Examples of reparative strategies might include customized care plans in maternity health care settings, but may also be focused on physical, psychological, and social environments.”
Long-term health of women and girls
The series, titled “Maternal health in the perinatal period and beyond,” calls for greater attention to the long-term health of women and girls—after and also before pregnancy.
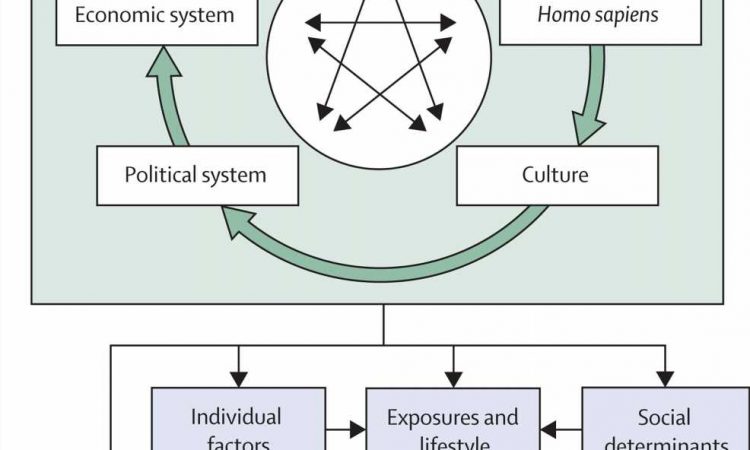
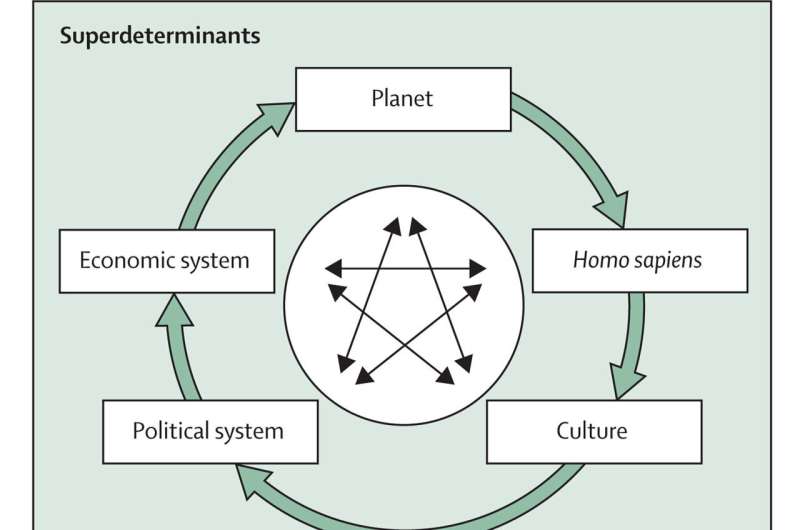
According to its opening paper published in The Lancet Global Health, a holistic approach is needed to reduce maternal deaths, focusing not only on their immediate biomedical causes but also on the complex interplay of broader social, economic and environmental conditions that affect women’s health, including racial and gender inequities as well as economic context, nutrition, sanitation, environmental risks, or exposures to violence and conflict.
Lack of attention to such fundamental issues helps explain why 121 out of 185 countries have failed to significantly progress in reducing maternal deaths over the past two decades, the paper contends.
Joao Paulo Souza, Centre Director of the Latin American and Caribbean Center on Health Sciences Information (BIREME) for PAHO/WHO and one of the authors of the first paper, said, “Maternal health is not just something that we should start worrying about when the pregnancy bump appears.”
“There are many factors that influence the likelihood a woman will have a healthy pregnancy, from the environment around her to the political and economic systems she lives in, or access to nutritious food and the level of agency she has over her life—all of these need to be addressed to improve her health, alongside access to high-quality health care throughout life.”
The series argues for a strong, multidisciplinary health system that not only provides high-quality, respectful maternity services but also prevents ill health and mitigates the impact of broader inequities—including specific interventions that support the most vulnerable women and girls.
More information:
Jameela Sheikh et al, Vulnerabilities and reparative strategies during pregnancy, childbirth, and the postpartum period: moving from rhetoric to action, eClinicalMedicine (2023). DOI: 10.1016/j.eclinm.2023.102264
João Paulo Souza et al, A global analysis of the determinants of maternal health and transitions in maternal mortality, The Lancet Global Health (2023). DOI: 10.1016/S2214-109X(23)00468-0
Source: Read Full Article